Chiropractic for Herniated Neck Discs works BETTER Than Medical Injections
Now this is the technical summary for a research paper published in peer-reviewed scientific journal but you can handle it!
Dr D
____
85.7% decrease in pain with spinal adjustments
25% decrease in pain with injection therapy
By: Mark Studin DC, FASBE(C), DAAPM, DAAMLP
Mark C. Zientek, DC DAAMLP, CHCQM
William J. Owens DC, DAAMLP
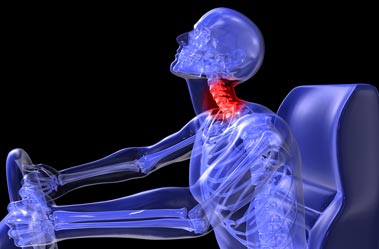
There is a large portion of the population who are dealing with various pain syndromes which includes neck pain from cervical disc herniations. According to Peterson, Schmid, Leemann, Anklin, and Humphreys (2013), this occurs in 83.2 out of every 100,000 people where symptoms range from mild to severe, but all negatively affect a person’s quality of life. To improve one’s quality of life, it becomes necessary to choose ways to manage and alleviate pain while reducing the side-effects of the actual treatment. Common methods range from simple masking of symptoms with over-the-counter medications to prescription opiates and invasive surgeries. Most people look for ways to manage pain and return to daily living activities without risky procedures and their inherent complications.
The use of over-the-counter medications and narcotics such as codeine and/or an oxycodone-acetaminophen combination like Percocet, is a common form of treatment by many primary care physicians and medical specialists alike. Kuehn (2013) reported:
“The FDA is concerned about inappropriate use of [opioid pain medications], which has reached epidemic proportions in the United States,” said FDA Commissioner Margaret A. Hamburg, MD, during a press briefing in September.
There was a 300% increase in prescribing of opioid pain medications between 1999 and 2010, a period in which the number of painkiller overdose deaths among women increased 5-fold and the number of such overdose deaths among men increased 3.6 times, according to the Centers for Disease Control and Prevention (MMWR Morb Mortal Wkly Rep. 2013:62[26];537-542). In 2010 alone, more than 15,000 US deaths were attributed to drug overdoses, and of the 10,000 overdose deaths in which a drug was identified, nearly two-thirds involved opioid pain medications…
The announcement comes after growing calls for the agency to tighten restrictions on the use of these drugs. In July 2012, Physicians for Responsible Opioid Prescribing (PROP), a group that includes prominent specialists in addiction, public health, emergency medicine, and pain medicine, petitioned the FDA to change the labeling for this class of drugs to discourage inappropriate use (Kuehn BM.JAMA. 2012;308[12]:1194-1196). The group argued that the drugs’ indications were overly broad and not consistent with the evidence base and may have been facilitating marketing for broader use than was appropriate. Specifically, the group argued that the agency should drop moderate chronic non-cancer pain as an indication, set a maximum daily dose, and add a maximum duration of use of 90 days. (p. 1547).
The problem, as acknowledged by the FDA, is that the AMA and many in medical academia appear to concur with the addictive qualities of the medications. The alternative option is the chiropractic spinal adjustment and it has been concluded in scientific outcomes to be a superior avenue for the relief of pain and reduction of disability with few side effects.
The earlier discussed study by Peterson et al. (2013) has confirmed that spinal adjustments (manipulations) provide significant improvement for patients with neck pain from cervical herniated discs, as well as arm pain (cervical radiculopathy) without the inclusion of opiates or surgery. In addition, this improvement was seen at all times, particularly at 3 months. In addition, in this Swiss study, it was found that the presence of radiating arm pain (radiculopathy) was not a contraindication to chiropractic treatment nor was it a negative forecaster of outcomes.
This study also found that with cervical herniated discs with radiculopathy, 85.7% of the patients experiencing acute pain reported significant improvement by three months with no patients being worse. For the sub-acute patients, 76.2% reported significant improvement by three months with no patients being worse with their disability indexes which were reduced from the onset of chiropractic care.
Another form of treatment for neck and arm pain commonly used is cervical spinal injections. In the same study compares cervical injection provided a 25% reduction in patients’ symptoms. The results of this current study of spinal adjustment (manipulation) treatments had substantially better results with more than 85% of acute patients and 76% of sub-acute patient improving, with a 65% reduction in arm pain as well as 59% reduction in neck pain at three months.
Chiropractic is one of the safest treatments currently available in healthcare and when there is a treatment where the potential for benefits far outweighs any risk, it deserves serious consideration, particularly as a first line treatment. Whedon, Mackenzie, Phillips, and Lurie (2015) based their study on 6,669,603 subjects after the unqualified subjects had been removed from the study and accounted for 24,068,808 office visits. They concluded, “No mechanism by which SM [spinal manipulation] induces injury in normal healthy tissues has been identified” (Whedon et al., 2015, p. 265). One risk factor for chiropractic care is a disc herniation. A properly credentialed chiropractor who has been trained to differentially diagnose and appropriately triage the patient is clinically indicated in this population of patients. The chiropractor can engage in co-management with medical specialists.
To best serve patients, a clear understanding of the outcomes and risks of procedures becomes necessary. Further research into the efficacy of chiropractic manipulation provides a clearly safe and effective treatment to the above-referenced condition. Examination of the research provides insight of avenues for relief of symptoms upon which physicians can undoubtedly rely.
Reference:
1. Peterson, C. K., Schmid, C., Leemann, S., Anklin, B., & Humphreys, B. K. (2013). Outcomes from magnetic resonance imaging–confirmed symptomatic cervical disk herniation patients treated with high-velocity, low-amplitude spinal manipulative therapy: A prospective cohort study with 3-month follow-up. Journal of Manipulative and Physiological Therapeutics, 36(8), 461-467
2. Kuehn, B. M. (2013). FDA tightens indications for using long-acting and extended-release opioids to treat chronic pain.The Journal of the American Medical Association, 310(15), 1547-1548.
3. Whedon, J. M., Mackenzie, T. A., Phillips, R. B., & Lurie, J. D. (2015). Risk of traumatic injury associated with chiropractic spinal manipulation in Medicare Part B beneficiaries aged 66-69 years. Spine, 40(4), 264-270.

Superb blog! Do you have any tips and hints for
aspiring writers? I’m hoping to start my own site soon but
I’m a little lost on everything. Would you advise starting with a free platform like WordPress or go for a paid option? There
are so many options out there that I’m totally overwhelmed ..
Any suggestions? Thank you!
Just start writing and pay attention to good grammar.
Hi mates, its impressive post on the topic of tutoring and entirely explained,
keep it up all the time.
I usually do not write many comments, but i did a few searching and wound up
here Cervical Disc Herniation with Radiculopathy (Arm
Pain): Chiropractic Care vs. Injection Therapy | Life Enhancing Chiropractic Care Center.
And I do have a couple of questions for you if you do not mind.
Could it be only me or does it look as if like some of the remarks
look as if they are written by brain dead visitors?
😛 And, if you are posting on additional sites, I’d like to keep up with everything new you have to post.
Could you list of all of your community pages like
your Facebook page, twitter feed, or linkedin profile?
sure,
Facebook.com/drdsays
twitter, @DrDRadio
LinkedIn, Dr. Demetrios Kydonieus
http://www.DrDSays.net
for my hobbies, fishing. http://www.snakeheadfishing.net
great issues altogether, you just gained a new reader.
What may you suggest about your post that
you made a few days ago? Any sure?
what post are you referring to?